Do you think you have fibromyalgia? Are you getting frustrated living in pain and getting no answers? The truth is, diagnosing fibromyalgia is a long and difficult process. On average, it takes over 2 years. Most people see three or more doctors before finally getting a diagnosis. Even with a doctor who is very experienced with fibromyalgia, diagnosis takes time.

Fibromyalgia is one of the most common types of chronic pain disorders. Awareness of fibromyalgia has increased and it has been accepted as a legitimate medical condition. Yet, fibromyalgia continues to be a hard-to-diagnose condition.
Why Diagnosing Fibromyalgia Is A Difficult And Long Process
There are several reasons a diagnosis of fibromyalgia is so tricky. For one, there is no lab test to rule out or diagnose fibromyalgia. Because there is no test for fibromyalgia, your doctor must rely on your symptoms to make a diagnosis.
The problem is the symptoms of fibromyalgia are common in many other health conditions. To make things, even more, confusing, fibromyalgia symptoms vary from person to person. And they tend to wax and wane in severity.
So, it’s important to determine whether your symptoms are caused by fibromyalgia or some other health problem. That’s why it can take a long time to get a fibromyalgia diagnosis.
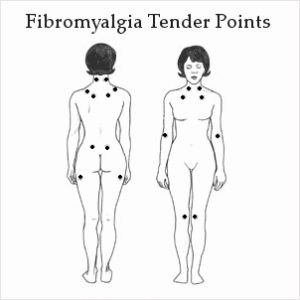
Tender Points
In the past, a tender point examination was used to diagnose fibromyalgia. Tender points are small areas on the body that tend to be painful when pressure is applied. Although a tender point exam is no longer a part of the FM diagnostic criteria, they are still an important characteristic of fibromyalgia.
There are 18 tender points. They are located on the neck, back, chest, elbows, hips, buttocks, and knees.
To get a fibromyalgia diagnosis, you had to feel pain in 11 of the 18 tender points when a doctor applied a certain amount of pressure. But there are a few problems when using tender points in diagnosing fibromyalgia.
First of all, fibromyalgia pain tends to wax and wane. You could have 11 tender spots on a bad day but only 7 or 8 on a good day. Secondly, tender point examinations were often done incorrectly. Many doctors weren’t sure how much pressure to apply and some avoided the exam entirely.
Doctors started taking into account other symptoms when diagnosing fibromyalgia. These symptoms include sleeping problems, cognitive difficulties, and impairment of daily living. But there was no set standard in place for diagnosing fibromyalgia. Many cases of fibromyalgia were going undiagnosed and/or misdiagnosed.
New Fibromyalgia Diagnostic Criteria
In 2010, the American College of Rheumatology released new FM diagnostic criteria. The new criteria intended to create a uniform standard used in diagnosing fibromyalgia. The new criteria, modified in 2011, consists of two main components in the clinical diagnosis of fibromyalgia:
- Ruling out other causes for your symptoms
- 6 self-reported symptoms and the severity of those symptoms
Ruling Out Other Causes For Your Symptoms
The symptoms of fibromyalgia are similar to those in various other health conditions. So doctors need to rule out other conditions first, before diagnosing fibromyalgia. These conditions may include hypothyroidism, rheumatoid arthritis, lupus, infections, and many others.
Ruling out other health conditions can take a long time and require seeing multiple doctors. The problem is that many people have coexisting conditions along with fibromyalgia. So a diagnosis of another health condition does not rule out a fibromyalgia diagnosis.
Since several conditions may coexist with fibromyalgia, it makes getting an accurate diagnosis, even more difficult. It is estimated that more than half of those with fibromyalgia have 5 or more chronic conditions, along with fibromyalgia. Some of these coexisting conditions include irritable bowel syndrome, depression, migraine, chronic headache, and anxiety.
It can take a long time to weed out whether these conditions either exist on their own or are simply a part of fibromyalgia syndrome.
Self-reported Symptoms & Symptom Severity
Although chronic widespread pain is the hallmark of FM, core symptoms of FM also include sleep disturbance, fatigue, mood disorders, headaches, and digestive problems. These core symptoms are now included in the diagnostic criteria. The 6 self-reported symptoms that are taken into account when diagnosing fibromyalgia include:
- Difficulty sleeping
- Fatigue
- Poor cognition
- Headaches
- Depression
- Abdominal pain.
The diagnostic criteria also includes 2 new methods of assessment:
- Widespread Pain Index (WPI)
- Symptom Severity (SS) scale
The Widespread Pain Index
The Widespread Pain Index lists 19 specific areas of the body. You determine your WPI score by counting the number of areas on the body where you have felt pain in the last week. You score 1 point for each area, so your possible score is between 0 and 19.
| LEFT | TRUNK | RIGHT |
|---|---|---|
| Jaw | Neck | Jaw |
| Shoulder | Chest | Shoulder |
| Upper Arm | Abdomen | Upper Arm |
| Lower Arm | Upper Back | Lower Arm |
| Hip | Lower Back | Hip |
| Upper Leg | Upper Leg | |
| Lower Leg | Lower Leg |
Symptom Severity Scale
There are 2 parts to accessing symptom severity. You will be asked to rate the severity of symptoms in four categories unrelated to pain.
First, you will be asked to rate these three symptoms:
- Fatigue
- Waking unrefreshed
- Cognitive symptoms: Trouble thinking or remembering
For each of the three symptoms above you rate the severity over the past 7 days based on the following scale:
- 0=No problem
- 1=Mild: generally mild or intermittent problems
- 2=Moderate: considerable problems and/or often present
- 3=Severe: pervasive, continuous life disturbing problems
So for part 1 of the Symptom Severity score, you have a possible 0 to 9 score.
For the second part of the SS score, you check off any somatic (physical) symptoms you have experienced. These symptoms include:
- Muscle pain
- Muscle weakness
- Irritable bowel syndrome
- Fatigue/tiredness
- Thinking or remembering problems
- Headache
- Pain/cramps in the abdomen
- Numbness/tingling
- Dizziness
- Insomnia
- Depression
- Constipation
- Pain in the upper abdomen
- Nausea
- Nervousness
- Chest pain
- Blurred vision
- Diarrhea
- Dry mouth
- Fever
- Itching
- Wheezing
- Raynaud’s phenomenon
- Hives/welts
- Ringing in ears
- Vomiting
- Heartburn
- Mouth sores
- Loss of/change in taste
- Seizures
- Dry eyes
- Shortness of breath
- Loss of appetite
- Rash
- Sun sensitivity
- Easy bruising
- Frequent urination
- Painful urination
- Bladder spasms
- Hearing difficulties
If you experienced none of the above symptoms, your score is 0. If you have 1 to 10 symptoms, your score is 1. 11 to 24 symptoms, your score is 2. And if you’ve had 25 or more symptoms your score is 3.
Now add part 1 and 2 together. This is your total Symptom Severity score, which can range from 0 to 12.
Then the WPI and SS scores are combined
A patient satisfies the diagnostic criteria for fibromyalgia if the following 3 conditions are met:
- WPI of 7 or higher and SS of 5 or higher or WPI of 3 to 6 and SS of 9 or higher
- Symptoms have been present at a similar level for at least 3 months
- If a patient does not have another disorder that would explain the pain
What About The New FM/a Blood Test?
There is a blood test that measures the level of cytokines, a protein molecule produced by a certain white blood cell. People with fibromyalgia have fewer cytokines in their blood than healthy people. The FM/a test is claimed to be 99% accurate. But critics argue that the same immune system markers can be found in people with other illnesses, making the FM/a test meaningless.
Anyone can request the test at www.TheFibromyalgiaTest.com. You have to fill out a questionnaire to see if you qualify for the test. Once you qualify, arrangements can be made to take the test through your healthcare provider or independently. The test costs over $700 and is generally not covered by health insurance, although that is starting to change.
Conclusion
Living with pain and not knowing why can be very frustrating. Until there are mainstream lab tests for diagnosing fibromyalgia, it will remain a diagnosis of exclusion. Since there are many other conditions that have similar symptoms, the process of elimination can take a long time.
Your doctor also has to rely on your description of your symptoms. Fibromyalgia pain can be hard to describe. There are different types of pain associated with fibromyalgia. The intensity of the pain can change from day-to-day. And the pain may move around or seem everywhere at once. You may struggle to accurately describe your pain to your doctor.
So, What Can You Do?
The most important thing you can do is to keep track of all your symptoms. Write them down. Take note of what activities, if any, that cause your symptoms to worsen. Also, take note of how your symptoms impact your life. You can use this Widespread Pain Index and Symptom Severity pdf document as a guide. It will show you what your doctor needs to know.
Remember to take your notes with you to all of your doctor appointments. This will help you clearly explain your symptoms to your doctor and hopefully lead to an accurate and timely diagnosis.
If you have any questions, ask in the comments below or use my contact form. I am happy to help in whatever way I can.



Is there any research explaining why severe fibro body pain completely stops when patient has a virus (throat/ears/nasal)?
None that I could find. Usually, fibro pain is worse when you have a virus.
Interestingly, I posted this oddity on some facebook fibro groups, and it seems its happened to others other than myself. Isnt this strange?? Im curious if there is a connection, virus vs virus, or something. Im not “science-minded” enough to figure it out or put it together.
Yes, it is strange. I guess that is why it is so hard to figure out what is really going on with fibro. We all experience commonalities and at the same time, it affects us differently.